In this special interest section we take a deeper look at some of the special needs, conditions, and considerations that are common in babies and young children. Please check back often as we continue to add to this page and update the content.
Congenital Heart Defects:
 Dr. Devyani Chowdhury, Board Certified Pediatrician and Pediatric Cardiologist weighs in about congenital heart defects.
Dr. Devyani Chowdhury, Board Certified Pediatrician and Pediatric Cardiologist weighs in about congenital heart defects.
Congenital heart defects are defects in the development of the heart. These defects are as common as 8 children born with a defect per 1,000 live births. Approximately 1% of children may be born with congenital defects in the heart; half of which will require some treatment. About 25% of these defects are critical and require an intervention in the first month of life. Some can spontaneously get better.
50% of major congenital heart defects can be detected with a fetal ultrasound of the heart. Some of these defects may be so critical that they require the baby to be born in a facility that can offer urgent cardiac interventions.
At birth, your baby’s oxygen level is checked. If the oxygen level is low it maybe indicative of a congenital defect in the heart. All babies in the State of Pennsylvania are required to have the oxygen level checked at birth.
Congenital heart defects can be treated by heart surgery or at times by performing a procedure like ballooning of the heart valve in the cardiac catheterization laboratory. Survival after interventions for simple heart defects is close to the normal population. The children with single ventricle are among the most complex and the overall survival of patients may be less than the general population.
A baby may present with poor feeding, low oxygen levels, breathing difficulty or poor weight gain as a sign of having a congenital heart defect. An older child would present with a heart murmur, or passing out, or symptoms with exercise. If there is any concern, it is important to discuss this with your family doctor.

Some congenital heart defects can run in families, such as problems with the left side of the heart. In certain genetic
conditions, such as Down Syndrome, there is a greater probability of having heart defects. If your child is diagnosed with a genetic condition, it is important to check with your doctor to determine if there are any associated heart defects with the condition. Sometimes maternal use of medications or illnesses in mother, such as Rubella, can cause congenital heart defects. Although there are many probable reasons for a child having a congenital heart defect, it is difficult to pinpoint the exact reason why a child has a congenital defect.
If your child is diagnosed with congenital heart defect it maybe helpful to connect with other families with children with heart defects or with support groups. There are many resources available and remember that you are not alone.
Q & A with Dr. Chowdhury:
- What are the most common congenital heart defects? The most common congenital defects (CHD) are the defects in the wall separating the chambers of the heart. These are also called as “holes” in the heart. A defect in the lower chamber of the heart is called a ventricular septal defect (VSD) and those in the top chamber are called atrial septal defect (ASD).
- What are the most common symptoms of congenital heart defects? The symptoms of the CHD depends on the age of the child. Most of the major CHD present in the first year of life. The common symptoms in a baby are poor feeding, poor weight gain, breathing fast and even turning blue with crying. In an older child it could be decreased exercise tolerance, passing out with exercise or poor weight gain.
- How is it diagnosed? Many CHD are associated with finding of a heart murmur. This is often heard by the child’s family doctor. A referral to a specialist, pediatric cardiologists is made. The pediatric cardiologist performs other initial tests like EKG (to look at the heart rhythm) or an echocardiogram (sonogram of the heart) to look at any problems in the structure of the heart. In addition, family history is very important in diagnosing genetic or familial conditions.
- How do you prepare parents emotionally for their children to have cardiac surgery? Cardiac surgery in a child is often a very traumatic event for the parents. It is emotionally draining to see your child go through heart surgery. I try to explain the defect and what needs to be done and answer all their questions. We also try to connect families with others who have gone through a similar surgery. We connect the family to the hospital social worker so some of the other needs during this time can be addressed. I strongly encourage families to discuss this issue with their cardiologist and family doctors as this is a big stress on the entire family. Please reach out to your support system when your child is undergoing cardiac surgery.
Plagiocephaly (Flat Head Syndrome) and Torticollis (tightness of neck muscles):
 By Dr. Aimee Ketchum, OTD, OTR/L, Pediatric Occupational Therapist
By Dr. Aimee Ketchum, OTD, OTR/L, Pediatric Occupational Therapist
Personally, I think there is nothing cuter than a baby in a helmet, but if we can prevent the need for one, we probably should go that route…plagiocephaly, or flat head syndrome occurs from positioning in the utero or positioning after birth. It is often called positional plagiocephaly. When there is repeated pressure on one spot of the skull, plagiocephaly can occur. It is very common and also, very treatable. Because newborn babies have a malleable skull, meaning they have soft spots and bones that are not completely fused yet, the skull can be formed into shapes other than round fairly easily. The purpose for the malleable skull is to allow for growth. Your baby’s brain will literally double in weight in one year due to new synapses between neurons if they get plenty of stimulation. The un-fused skull allows for this growth, but can also allow for a mis-shaped head when too much pressure is on one specific area. The best way to assess the shape of your baby’s head is to look at it from the top. It is important to note that one reason for the malleable skull is to allow the baby through the birth canal. Don’t be alarmed if your baby’s head is shaped like a cone when they are born vaginally. This is not plagiocephaly, it is simply due to the pressure of the birth canal and this will typically resolve within a few days or weeks at the most. It is also important to note that plagiocephaly does not affect the child’s mental development, as the brain is very protected.
Babies with plagiocephaly may have a secondary condition called torticollis. This is a tightness of one side of your baby’s neck muscles. This is often caused by position in the utero and you can identify this by noting how your baby turns his head. Does he always look one direction and does it seem like his neck is stiff and uncomfortable if you try to turn his head the other way. This contributes largely to plagiocephaly and if you suspect this, you should let your baby’s healthcare provider know right away because he may require occupational therapy or physical therapy to release those tight muscles and work on positioning.
Premature babies are at higher risk for plagiocephaly because they often spend extended periods of time in one position in an incubator in the NICU.
In 1992 the American Academy of Pediatrics came out with the recommendation that all babies sleep on their backs in the  “Back to Sleep Campaign” to decrease the chance of sudden infant death syndrome (SIDS). While the incidence of SIDS decreased, the incidence of positional plagiocephaly dramatically increased.
“Back to Sleep Campaign” to decrease the chance of sudden infant death syndrome (SIDS). While the incidence of SIDS decreased, the incidence of positional plagiocephaly dramatically increased.
Let’s talk about treatment first, then I will talk about what parents can do to prevent plagiocephaly. Once your child is able to sit and stand, the prolonged pressure on his head is mostly eliminated and the head will become more round naturally, then their hair will cover any remaining flat spots. For pre-term babies and very young babies a gel pillow can be utilized to decrease the pressure on the skull. Another option is the Tortle which is a hat that prevents the baby from turning his head so that pressure is not allowed on the flattened part of the skull. If changing the baby’s positioning, and use of a gel pillow and Tortle is not effective and your baby’s child care provider diagnoses your baby with plagiocephaly, they may refer your baby to a pediatric neurosurgeon. The pediatric neurosurgeon will fully evaluate your child, take specific measurements and possibly refer your baby to an orthotist. The orthotist will probably make a mold of your child’s head and fabricate a helmet that is customized to your baby’s head and specifically designed to achieve symmetry. According to the American Association of Neurological Surgeons, helmets are most effective between three and six months, but correction is still possible up to 18 months, it might just be a longer process. It will be recommended that your baby wear the helmet at all times, removing it only for baths.
Prevention of plagiocephaly:
- Allow your baby lots of supervised tummy time from the day she is born. We recommend 5 minutes several times per day as newborns and up to 20 minutes a few times per day for three-month-old babies.

- Carry your baby in vertical baby carriers and slings. This relieves pressure from your baby’s head and also has the added benefit of keeping your baby close to you to help with bonding, learning new language, and processing the world from the vertical position, building balance and equilibrium.
- Hold your baby upright on your shoulder whenever possible.
- Move baby’s mobile from one side of the crib to the other side, so your baby is gazing up at it from alternate directions, changing the position of your baby’s head
- When holding your baby and feeding your baby, try to change position from right side to the left side so pressure on his head is symmetrical. This is also great for your baby’s developing vision.
- Re-arrange your baby’s room or the position of her crib or bassinet, so she looks in a different direction. Babies typically look toward the light source or toward the door, anticipating you coming in.
- Try to eliminate time spent in baby carriers, car-seats, and bouncy seats. Hold your baby or use a baby carrier whenever possible. Try to leave the carseat in the car.
Remember, plagiocephaly is very common and very treatable, but it is important to get intervention quickly. Don’t wait and hope that it resolves on its own.
Hip Dysplasia:
 Pediatric Physical Therapist, Dr. Tanya Myers weighs in about hip dysplasia.
Pediatric Physical Therapist, Dr. Tanya Myers weighs in about hip dysplasia.
As parents, we worry about everything. Has the baby eaten enough? Are they sleeping too much? Mothers are juggling so many things and they often worry too much. It is with great caution that I write this piece about hip dysplasia, but I want you to be educated and avoid using the many things on the internet that could cause more concern.
Hip dysplasia means that the hips are not forming in a typical manner. The cup or socket (pelvis) that the thigh bone (femur) sits in is too shallow and the top of the hip bone can be abnormally shaped. Therefore, the hips, or head of the femur slips out of the socket. In all babies, the hip is not fully developed at birth, but as the baby grows, and puts weight on the legs, the socket becomes deeper and the hip bone changes shape to fit nicely in the socket. When the socket or hip bones are not in the correct position, the bones slip apart and they do not form into the correct shape. Now sometimes if it is minor enough, things turn out ok and no noticeable problem occurs. However, sometimes the bones need a bit more help so that the child can walk and run without noticeable problems. Often times, the hips are moved into the correct position with use of a splint. 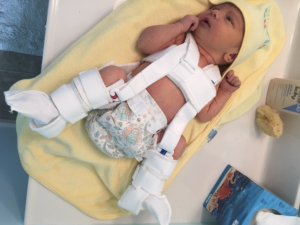 Hip dysplasia can be diagnosed at any age. When it is diagnosed in infancy, you may notice that one leg is longer than another, the hips click during diaper changes, or one leg is less flexible than the other. It can affect one or both legs.
Hip dysplasia can be diagnosed at any age. When it is diagnosed in infancy, you may notice that one leg is longer than another, the hips click during diaper changes, or one leg is less flexible than the other. It can affect one or both legs.
Now you might wonder why or how this occurs. Sometimes, we do not know but factors that may play a role include positioning in the womb, being a first child, or being born head first. It occurs more often in girls versus boys. Your baby will be checked shortly after birth and during “well child” visits. If you have concerns, never hesitate to ask your child’s doctor. This condition is usually not painful for the infants. The doctor will usually do a quick test called the Bartow’s and Otolani test. This includes moving the hips around to check for a click or dislocation. If they notice any problems, the doctor will order an x-ray or ultrasound. Treatment will then depend on the severity and the age of the child. Sometimes, it is just a wait and watch situation and other times a harness, called the Pavlik harness is worn for several months. The harness holds the hip in alignment as the socket develops. Sometimes more aggressive procedures are required such as surgery or casting. Pediatric physical therapists can be helpful in providing care for these kids. One of the most important things is that you keep in contact with your child’s doctor and follow their instructions. Never hesitate to ask questions and seek a second opinion if needed.
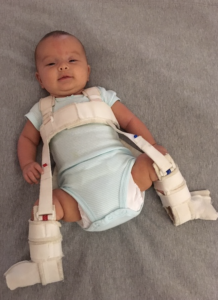
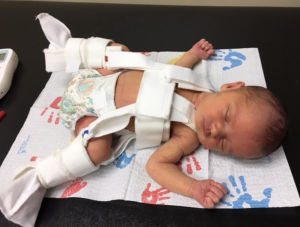 Because I think parent’s often have the best advice for each other, I am also
Because I think parent’s often have the best advice for each other, I am also
including a parent’s top 10 tips. Erin Whiskeyman has been providing support for her daughter Paisley who has had this condition in both hips since birth. She used a Pavlik Harness for several months and is currently being seen for Physical Therapy treatment and walking like a champion. As of this writing she is now about 1.5 years old and a happy an independent little girl .
Here is Erin’s advice and some great pictures of Paisley:
- Feel all the emotions. Having a baby fitted and placed immediately into a brace is so overwhelming. Let yourself feel sad and grieve the losses that barrier will have on their babyhood moments.
- Educate yourself. Learn about the causes, treatments, terminology, and outcomes for the diagnosis. You’ll feel more confident at appointments, be able to ask meaningful questions, and be more engaged in the process.
- Find support. Facebook has great parent groups where you can ask questions, seek advice, and validate your emotions along with other families who are in your shoes. This is much more common then you would ever imagine.
- Be creative with clothing. 24/7 brace wearing doesn’t allow for cute clothing options. Side-snap shirts, oversized dresses and t-shirts, leg warmers, and wide sleep sacks are great!
- Embrace the grime. The braces get dirty even when your careful. Spot clean only as needed.
- Verify your baby gear. There are a lot of baby accessories that do not promote healthy hip development; swaddles and wraps, Bumbo chairs, jumpers, walkers, and so on. Check first before you use any movement or carrying related equipment. There are many popular baby wearing carrier options that are deamed hip healthy!
- Stick with it. Tummy time, breastfeeding, cloth diapering, baby wearing can all be done successfully. However, there is more of a learning curve as everyone involved gets used to the extra brace bulk.
- Trust the process. This is a common diagnosis, which many doctors are familiar with, and even though severity and treatments can vary, the diagnosis also comes with high success rates.
- Remember, despite how terrifying that “click” or “clunk” may feel, it’s doesn’t cause discomfort or pain to the child. You will not hurt them as you are moving them.
Some Additional References:
https://www.mayoclinic.org/diseases-conditions/hip-dysplasia/symptoms-causes/syc-20350209
https://hipdysplasia.org/developmental-dysplasia-of-the-hip/causes-of-ddh/


